Information Leaflet
Benign Breast Conditions
The majority of breast referrals—approximately 85%—are for benign conditions rather than cancer.
While symptoms such as pain or lumpiness are often harmless, thorough investigation is essential to rule out serious causes and provide appropriate care. The links below offer trusted information on common benign breast conditions, helping you make informed decisions about your health. For more information please visit Breast Cancer Now Website.
Breast Cancer and Treatments
Breast Health
Breast health begins with understanding what is normal for your own breasts—often referred to as breast awareness. Regular breast self-examination can help you become familiar with natural changes in sensitivity and texture, which may vary at different times during your menstrual cycle. Many women have concerns about breast lumps, pain, or nipple discharge. Knowing what is normal and recognising when to seek medical advice is an important part of breast care. It is also helpful to understand common screening and diagnostic tests, including clinical breast examinations, mammograms, and breast ultrasounds. This page has been designed to provide you with the information you may need—simply click on the links below to learn more.
Cosmetic Surgery
Abdominoplasty (tummy-tuck)
What is an Abdominoplasty?
Click here for BAAPS information for patients
Abdominoplasty, commonly known as a “tummy tuck” or abdominal resection, is a major surgical procedure designed to rejuvenate the abdominal area by removing excess skin and fat. It is often performed for patients who have experienced significant weight loss or to address loose tissue following childbirth. In most cases, the procedure also restores weakened or separated abdominal muscles, resulting in a firmer and more contoured abdomen. Repositioning of the umbilicus (belly button) is usually required. An abdominoplasty will leave a scar extending from hip to hip, as well as a scar around the umbilicus. The operation is performed under a general anaesthetic. For further information, please visit the BAPRAS website using the link below.
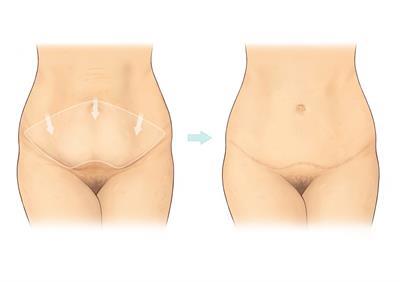
Why am I having an Abdominoplasty?
- An abdominoplasty reduces excess skin from your abdomen following major weight loss
- After successful treatment for obesity or following pregnancy.
- It may also help to tighten abdominal muscles, which have become weakened over a period of time.
What are the alternatives?
There are no alternative treatments which the surgeons can offer you.
Who is unsuitable for a tummy tuck?
Those who have been encouraged to improve their body contour by others. Abdominoplasty surgery is not recommended to people with unrealistic expectations, smokers and those with a significant medical history i.e. diabetes, cardiovascular disease, immunosuppressed. If you plan to have more children, you should consider having them prior to surgery.
What are the risks associated with an Abdominoplasty?
In the majority of cases this operation is carried out very successfully with good cosmetic results. However, as with any operation, there is a chance of side effects or complications. Below is a list of complications that can occur following an abdominoplasty. This list of complications is not intended to put you off having the operation but you need to be aware of any potential complications before you consent to having surgery.
- Bleeding
During or soon after the operation you may experience bleeding from your wound, which can result in a collection of blood (called a haematoma) beneath the wound site. Should this occur you could experience excessive pain and swelling in your abdomen. Healthcare staff will assess this and will offer you painkillers to alleviate this. The collected blood may need to be removed in the operating theatre; this may mean having a further small procedure. Two drains will be required to help minimise the excess blood and fluid in the early post-operative period. These will be removed by a District Nurse or myself at your follow up.
- Loss of skin from your abdomen
During the operation cuts are made through the skin and fat of your abdomen. This tissue always requires a very good blood supply. Sometimes the blood supply to the skin is disrupted and becomes inadequate. This means some of your skin may not be viable causing another wound on the surface of your abdomen; (This is called skin necrosis). Should this happen, healing to your wound will be delayed and extra scarring may occur. A further implication of skin loss may be the need for further surgery to correct the problem. This may include vacuum dressings or a skin graft operation at a later date.
- Fat necrosis
Your abdomen contains large amounts of fatty tissue beneath the skin which can have a reduced blood supply after the operation and cause long term lumpiness and distortion.
- Chest infection
A chest infection can occur following any general anaesthetic. You can help to reduce the risk of this happening by taking regular deep breaths following surgery and getting up and sitting out of bed as soon as you are well enough. If you smoke or vape you can reduce the risk of a chest infection by stopping for at least six weeks prior to your operation.
- Anaesthetic risks and complications
Your operation will be carried under a general anaesthetic. Your anaesthetist will give you more information about your anaesthetic and will discuss anaesthetic risks and complications with you prior to your surgery following an assessment.
- Umbilical necrosis
During the operation your umbilicus (belly button) will need to be repositioned. There is a small risk that by repositioning the belly button all or part of the skin of your belly button to die. If this happens healing will be delayed and you may need another operation to correct the problem.
- Fluid collection beneath the wound
There is a risk that fluid may pool beneath your stitch line after surgery (this is called a seroma). A seroma can occur at any time after the operation. This fluid is usually re-absorbed by the body over a period of time. There are situations in which a doctor may need to remove the fluid using a small needle and syringe if the seroma causes pain and discomfort. In some cases the fluid can collect again so this procedure may need to be done more than once. This happens on occasions to other patients and the surgeon will discuss the risks of a seroma with you before your operation. As mentioned before two drains will be inserted to minimise seroma collection.
- Wound infection
A wound infection can occur at any time following surgery. If your wound becomes infected you may need treatment with antibiotics or you may require hospital admission for further surgery to drain and treat the infection. Signs and symptoms of wound infection can include increased swelling, redness, fluid leakage and increased pain in your abdomen.
- Wound breakdown
Wound breakdown can occur following surgery. Often there is some delay in healing of the stitch line. However; in rare cases the stitch line may not heal properly and the wound may breakdown or gape open. As a result, dressings will be required for prolonged periods and a further operation maybe needed to hasten healing and/or minimise the distortion that this complication can sometimes cause. If you smoke or vape you can reduce the risk of a chest infection by stopping for at least three months prior to your operation.
- Excess or abnormal scarring
You will have a permanent, scar on your skin. Your scar can be concealed by clothing, however this cannot be guaranteed by the types of clothing you decide to wear. Your scar can sometimes improve over a period of 18 months following surgery however; some people for unknown reasons, develop raised, red and lumpy scars. Unfortunately this is largely beyond the control of the surgeon. The chances of this occurring are greater if you have already developed thickened scars following accidents or operations elsewhere. Scars sometimes stretch as they mature and this is also largely beyond surgical control.
- Fat necrosis
During your operation cuts will be made through fat tissue. Rarely the blood supply to this area becomes disrupted, causing this tissue to become non viable. Should this happen the fatty tissue can become liquified and start to leak out of the wound (fat necrosis). This may mean having another operation to correct the cause and correct any deformities.
- Asymmetry of the umbilicus and scarring
During an abdominoplasty operation your surgeon will need to reposition your umbilicus (belly button). There is a risk that your umbilicus may not be placed centrally on your abdomen (as it was before your operation). Some degree of asymmetry of your scar may also be evident. If you are concerned about asymmetry after your scars have had at least 12 months to settle you should discuss this with your surgeon.
- Dog-ears
Once your wounds are healed you may notice an excess of skin at either end of the stitch line, these are known as dog-ears. If these have not settled down after 12 months, it is best to discuss further management with your surgeon. A further operation may be necessary to correct this.
- Altered sensation in your thigh and abdominal skin
You may experience some numbness in the lower part of your abdomen and thighs after this operation. In the majority of people this numbness reduces over a period of 12 months following surgery. Sometimes a small number of people may experience permanent numbness of their skin following abdominoplasty.
- Deep vein thrombosis (DVT)
This is a blood clot that arises in the deep veins of the leg or pelvis. A deep vein thrombosis can happen if your mobility is restricted or you are inactive for a time following your operation. You may be given injections that help to prevent this from happening. You can reduce the risk of deep vein thrombosis by wearing the elastic stockings supplied during and after your operation and moving your legs about whilst you are in bed. Getting up and walking as soon as you are well enough may also reduce the risk of a DVT.
- Pulmonary Embolism (PE)
This is a portion of blood clot that has become lodged in a small blood vessel in your lung. It can cut off some of the blood supply to your lung causing shortness of breath or pain when you breathe in deeply. PE is a serious complication of surgery. You can reduce the risk of PE by following the advice for the prevention of DVT listed above. Patients are offered injections which help thin the blood after their operation as mobility may be limited and this can sometimes predispose to a PE or DVT. If you take the oral contraceptive pill or HRT you may be contacted by the hospital and asked to stop taking them. If you do stop taking the contraceptive pill remember to use some other method of contraception to avoid pregnancy. If you do not hear from the hospital, then continue to take your medication as normal. You will be asked to attend a pre assessment clinic at Frimley Park Hospital. These investigations will include a blood test. Photographs may be taken of your abdomen for your medical records and you will be asked for permission for the photographs to be taken.
There may be other risks specific to your individual case. The surgeon or ward nurse will discuss any further risks with you.
How do I prepare for my operation?
Please be prepared to take up to four weeks off work to recuperate depending on your type of work.
If you are overweight you will be asked to reduce your weight to within normal limits for your height. You will need to achieve this weight reduction before admission to hospital. If you need help to reach your target weight your GP may be able to refer you to a dietician.
If your GP prescribes aspirin, ibuprofen or other medications which may cause bruising or bleeding such as clopidogrel or Vioxx, you may be asked to stop taking these for a period of seven days before your operation. These medications may increase the risk of bleeding during and after your operation. Your surgeon will advise you about this when you see him / her in clinic. If you do not hear from the hospital, then continue to take your medication as normal.
If you normally take warfarin tablets you may be asked to stop taking these 5 days before your operation. You may also be asked to have a blood test on the day of your operation.
What happens when I come into hospital?
A doctor will make sure that you are informed about the nature of your surgery and the possible complications. He or she will ask you to sign a consent form agreeing to the surgery. On the day of your operation you will need to stop eating and drinking for a period of time, the nursing staff will advise you of when this will be. Please have a bath or shower before your operation. If you have any questions or concerns about your operation please ask a member of the nursing staff for assistance.
What happens after the operation?
The operation will take about 1-2 hours to complete however; you will be in the operating department for longer than this to allow time for recovery. When you wake up from your operation you will be lying in a ‘jack-knifed’ position; this means that you will have pillows under your knees, keeping your hips and knees bent to reduce the tension on your abdomen. You will be asked to sleep with your hips and knees in this position for several days following your operation to reduce the strain on your stitches.
You should not lie on your sides or stomach as this will cause discomfort and will put pressure on your stitches.
Because of the increased risk of thromboembolism you will require calf compression devices, in addition, you will be injected daily with an anticoagulant under the skin which you will need to continue yourself for two weeks after surgery.
The nurse looking after you will regularly check your wound, your drains, your blood pressure and pulse after you return from theatre. You will not have a catheter in place. You will be able to eat, drink and mobilise as soon as the anaesthetic subsides.
There will be bruising, swelling and discomfort following your operation and you will be offered pain relief either by injections, tablets or a patient controlled pain relief pump.
You may have a drip, usually in your hand or arm, to replace any fluid lost during your operation. You may lose blood during your operation; sometimes you may need a blood transfusion to replace this. Alternatively, you may be prescribed iron tablets to correct any associated problems.
You will also have a dressing over your wound.
There will usually be a drain (tube) at either side of your abdomen, which drains away any excess blood into a bottle attached to the drain. These drains will be removed when there is only a small amount of drainage. This can take several days. Your dressing will normally be left in place for up to 10 days unless it becomes wet, in which case it may be changed earlier.
You are encouraged to get up on the day after your operation to help prevent the formation of any blood clots in your legs. You will be asked to walk in a ‘stooped’ position or with your back bent over for a few days to reduce the strain on your stitches.
How long will you stay in hospital?
Normally you can expect to be in hospital for 3-5 days after your operation; however this depends on when your drains are removed and the preferences of your surgeon.
What happens when I go home?
You are normally prescribed a weeks supply of painkillers to take home. If you need a further supply you should contact your own doctor. (GP)
When you are discharged from hospital you should keep fairly mobile but avoid any movements that cause straining or stretching to your abdominal muscles and wound.
You should arrange for a friend or family member to collect you when discharged and have some support at home for the next week. You do not need any special care at home, however if you have small children it may be advisable to arrange for someone to help you to care for them. Please do not use a hot water bottle to relieve abdominal discomfort at any time after your operation, as there is a chance this can damage your skin, as you may be numb in this area and be unaware of excessive heat. You can potentially leak very hot water onto your wound.
Follow up
Whilst in hospital you will be reviewed daily and will be discharged with your drains in place. The ward will arrange for District Nurse to visit you at home and measure your drain output daily. Your dressings will be changed after 7-10 days in clinic. Any staples or stitches will be removed in clinic, usually within two weeks of your operation.
You will have dissolving stitches that do not need to be removed. You will require dressings until your wounds have healed. Once your wounds have healed you should massage your scar regularly with a bland oily based cream such as bio oil or silicone gel/tape as this may help it to settle down and relieve itching. You will be sent an appointment to see your consultant in the out patients department at approximately 1-2 weeks following surgery.
What else can go wrong?
It is normal to have some bruising, swelling and tenderness around your abdomen for several weeks following the operation. However if you suffer from any of the following symptoms after your discharge from hospital you should telephone the numbers provided on your discharge summary for advice:
- Persistent or increasing levels of pain;
- Fever and increase in temperature
- A feeling of heat in your abdomen;
- Redness or swelling of your abdomen;
- Tiredness or fatigue that lasts longer than three weeks.
- Shortness of breath or pain when you breathe in deeply.
When can I resume normal activities again?
You should not drive until you can wear a seat belt comfortably and feel able to perform an emergency stop; this could be up to 6 weeks following surgery. Your insurance company may refuse to meet a claim if they feel you have driven too soon. It is also advisable to contact your insurance company with regards to cover following a general anaesthetic. You should not go back to work until instructed by your surgeon. This could be 4-6 weeks depending on your job. You will be given details on when you can resume activities. Please ask if you need a doctor’s certificate for your work, should you need follow up certificates you should see your GP. You may resume sporting activities approximately 6 weeks after your surgery; however you should stop if you experience pain or discomfort during the activity. Sexual activities can be resumed once your bruising and swelling have subsided however you can discuss this with the surgeon before your operation.
Please do not hesitate to ask any further questions at anytime, we would be more than happy to help.
Breast Augmentation
Implant type
There are both saline filled and silicone gel filled implants available. There is no evidence that silicon is harmful or can cause disease outside the breast, and most modern implants have an outer silicone shell even if they are filled with saline. Many implants are now made of “cohesive” silicone gel. While this feels soft, it has a structure like a jelly cube, so cannot leak out into the breast tissues as easily as the older liquid silicone implants.

Implant Size
The correct implant size depends on a combination of factors – your desired size after surgery, the size of your chest, whether your breast sit high up or lower down on your chest and your degree of ptosis. It is usually helpful if you can bring some pictures of women who have the sort of proportions and shape you wish to achieve, so we can agree on your aims. There is also a very useful technique you can use at home to try and work out how much larger you want to be.
Silicone shell sizers
During your consultation you will have the opportunity to see an approximation of your final result with the use of silicone shell sizers. You may find it useful to bring a non padded bra in your desired cup size to these consultations for this purpose.
Positioning of the implant
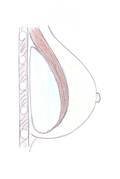
The implant can be placed directly under the breast in a subglandular position or under the muscle of chest wall, the subpectoral position. A technique known as the “dual-plane” can be used which combines the two, and may help correct ptosis while at the same time increasing tissue coverage over the upper part of the implant. Every woman obviously represents an individual case and we will discuss the various advantages and disadvantages of each approach for you personally.
The Operation
The operation is normally performed under a general anaesthetic. Various approaches are available for the placement of the implant. The commonest approach is by placing the scars underneath the breast in the breast crease. This is generally considered the one required for the placement of silicone gel implants as they do not compress enough to be squeezed through holes in either the armpit or around the nipple. The stitches used are dissolvable. The operation takes 1-2 hours and you will probably stay one night in hospital.
Following the procedure the wounds will be dressed with surgical glue and paper strips. This will allow you to shower and bath in the post-operative period as normal and should just need to be patted dry. Antibiotics are given during and sometimes after the operation to prevent infection.
Returning Home
You are likely to feel some discomfort for the first few weeks and you should avoid any heavy lifting or strenuous activity for 3-4 weeks. You should be able to drive after 2 weeks and most women can return to work by this time. You will be advised to wear a sports type bra (ideally front-fastening) for the first few weeks. You will be reviewed in clinic 2-3 weeks after the procedure
Breast Implant Associated Anaplastic Large Cell Lymphoma (BIA-ALCL)
Information for patients, public and health care professionals:
https://www.gov.uk/guidance/breast-implants-and-anaplastic-large-cell-lymphoma-alcl
Going abroad for cosmetic breast surgery?
Breast Reduction
Who chooses to have breast reduction?
Most women who desire a breast reduction simply feel that their breasts are disproportionately large and heavy. For many women this makes it difficult to find clothes which fit properly, particularly dresses. Some women with large breasts develop “shoulder grooving” from the bra straps, and rashes under the breasts in hot weather. Others complain of back and neck pain and feel that the heaviness of their breasts is causing postural problems.
Some women develop very large breasts during puberty; others find that their breast size increases after having children or following the menopause.
A breast reduction will not prevent breast pain, as there is still plenty of breast tissue left after the operation, but some patients find that the heaviness associated with their pain is better after surgery.
A breast reduction will not prevent you getting breast cancer, though there is some evidence that reducing the amount of breast tissue can reduce the risk of cancer slightly. It is important to remember that mammograms will be less accurate after a reduction because the scar tissue inside the breast can mask a very small cancer, and you should tell your mammographers that you have had reduction surgery.
For more information from the Association of Breast Surgery, BAPRAS and BAAPS websites on breast reduction.
Preoperative Assessment
During the initial consultation I will discuss with you your reasons for wanting a reduction, and how much smaller you would ideally like to be. It is not possible to guarantee a particular bra size afterwards, due to the different ways bra size is calculated. The procedure is designed to make your breasts proportionate with your trunk, so the final size will depend to some extent on your overall size.
I will discuss with you the risks and complications of breast reduction surgery and what to expect afterwards. You will be shown photographs of the procedure and the results. There are several different methods of performing a breast reduction and I will discuss which of these are appropriate for you.
If you are 40years or older a preoperative mammogram will be ordered.
Types of Breast Reduction
Although it is possible to reduce breast size in some women by liposuction alone, I do not generally advise this, as it dos not incorporate any form of uplift, and so does not give very good overall results.
In small-breasted women who need a small reduction in order to improve symmetry, then it is sometimes possible to use the Benelli technique, which leaves only a scar around the areola, the pigmented skin around the nipple. This type of reduction does not work for moderate or large breasts.
The commonest type of breast reduction performed in the UK is the inverted T, or Wise pattern, technique, which leaves a scar around the areola, down to the crease under the breast and along the crease from end to end. Like the Benelli, this technique is dependent on the breast skin to hold the shape of the breast. Over time, the skin tends to stretch and the breast “bottoms out”, leaving most of the breast tissue sitting below the level of the nipple, rather than behind it. In extreme cases, this can lead to difficulty wearing a bra, as the high-riding nipple is pushed out of the top of the bra cup.
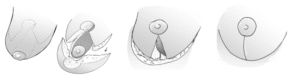
Post Operative
You can expect to stay in hospital for 1 night after the operation. You may require drains overnight which are typically removed before you go home. You are likely to experience some discomfort, but this can usually be controlled by normal painkillers. You will be sent home with antibiotics to take to prevent infections. It is recommended that you wear a sports bra day and night for 2 weeks after the operation and then during the day for a further 2 weeks
You are likely to have paper tape dressings over the wounds which should be left in place until you are seen in the clinic at around 1-2 weeks. These are showerproof and should simply be patted dry after bathing. They may start to look a little frayed by the time you come back to the clinic, but it is best to leave them in place for the first few weeks, rather than changing them.
You will be seen in the clinic 2-3 weeks after surgery, to check that your wounds have healed well and that you have developed no other problems. You will be advised to continue wearing the dressing tape for as much time as possible over the next 3 months, as this helps to keep your scars from widening. You can change the tapes yourself every week or so during this time. You will be seen again at 3 months and 1 year postoperatively.
Complications / Side Effects
Breast reduction surgery involves a general anaesthetic and takes 3 hours. The usual risks of a long operation are therefore present. These include both chest infection and deep vein thrombosis (clots in the legs that may spread to the lungs – pulmonary emboli, which whilst very rare, can prove fatal). Steps are taken to reduce the risks and these include the use of compression stocking and early mobilisation.
Sometimes bleeding occurs in the hours immediately after the operation. This usually makes one breast more swollen and uncomfortable than the other. Sometimes it is necessary to return to theatre to remove the haematoma (blood clot) and stop any further bleeding.
Nipple sensation
The nipples and breast will be numb after the operation. As sensation returns you may experience sharp shooting pains. Sometimes not all the sensation returns, particularly in the nipple, which may lose all or some of its sensitivity, including erotic sensation. Occasionally patients describe increased nipple sensitivity after breast reduction. These changes may not be symmetrical.
Nipple Necrosis
There is a very small possibility that the nipple may lose its blood supply and become necrotic (the skin may become black and heal by scarring with loss of pigmentation) or you may even lose the nipple in extreme cases. This is extremely rare. Nipple reconstruction can be performed at a later date, and loss of pigmentation can be corrected by tattooing.
Infection is another possibility despite the routine administration of antibiotics during the procedure. If you do get an infection, the scars can become a little thicker and the eventual scar you are left with may not be like the one you are shown pre-operatively. Even without infection some women develop thick unsightly scars due to a condition called keloid. Special silicone dressings may be required to treat these scars. The scars may also become quite broad.
Fat necrosis occurs when a part of the breast tissue that is left behind does not have a good enough blood supply. It usually takes the form of small lumps just beneath the scars which are noticed about 2-3 months after the operation. Rarely, a large area of the breast can go generally firm. The condition is benign and does not carry any risk of cancer, and often settles with time. Lumps that do not resolve can often be removed.
Returning Home
Once discharged home, you can bath or shower as normal. The stitches in your wound will dissolve. The dressings are left until the first clinic appointment. An appointment will be made for you to come back to clinic about 2 weeks after discharge. You can expect bruising and swelling in the breasts and will be hard and swollen for some weeks.
Lipofilling or Fat Transfer
Fat Transfer (Fat injection) to Breast
You are going to have structural fat transfer to the breast. This procedure is also referred to as ‘Fat injection’ or ‘Lipofilling’. This procedure has been performed worldwide for over twenty years. This leaflet explains what the procedure involves and some of the potential benefits and problems.
What is Fat injection and how is it performed?
This procedure involves taking fat tissue (liposuction) from your tummy wall, thighs or buttocks, preparing this tissue and then re-injecting it into your breast. Your surgeon will discuss with you the most appropriate place to take the fat from. The procedure is usually done under a general anaesthetic and you may need to stay overnight.
Who would benefit from Fat injections?
In our unit this procedure is usually performed in patients who have developed an indentation in the breast following lumpectomy and radiotherapy for breast cancer. We also use this technique in patients who have had breast reconstruction in whom the breast shape may be improved.
This procedure is also used in men who have developed a deformity after treatment for gynaecomastia (Enlargement of breasts in men). Worldwide, fat is being injected for cosmetic reasons into faces, hands and other areas of the body to improve appearance.
What are the benefits of Fat injection?
The benefit is to improve the appearance of the breast by reducing ‘dents’, replacing volume deficits and in some cases it improves skin appearances after radiotherapy.
What are the risks of Fat injections?
All operations carry some risks and fat injections can be associated with problems.
These include:
- Bleeding can occur at the site of liposuction or in your breast. This bleeding is called haematoma and sometimes a smaller operation would be needed to remove this blood.
- Bruising is common at the site of liposuction and occasionally in your breast. Bruising usually settles in a few weeks and does not require any specific treatment.
- Infection can occur at the site of liposuction or in your breast where the fat has been injected.
- The signs of infection are redness, swelling, increase in temperature and discomfort at the site of the wound infection. Should the wound get infected, you will be reviewed and given antibiotics if appropriate. Wound infection after fat injection treatment is uncommon and you will be given antibiotics at the time of your operation to reduce this risk.
- Pain can occur at the site of liposuction and should respond to painkillers that will be given at discharge. Injury to abdominal organs from liposuction to the abdomen may be a serious but very rare complication.
- Nerve injury; during liposuction, some of the nerves carrying sensation from the overlying skin may be damaged, and this could result in numbness which is usually temporary but can be permanent. Very rarely some patients may experience altered sensation called paraesthesia as a result of nerve damage.
- Some of the fat that has been injected into your breast may not survive and can die this is called fat necrosis. This may present as a lump in the breast and will be checked and treated by your specialist. Treatment sometimes involves removal with a needle and syringe.
- Repeat procedure: Sometimes the procedure needs to be repeated to achieve the desired effect.
- Stem cells; It is believed that some of the cells in fat have properties that allow improvement in your skin and tissue texture and form, this is one of the main reasons that this procedure is used cosmetically. It is unknown if these properties can have any negative effects on the risk of breast cancer recurrence, but to date no such problems have been recorded in the breast.
- Underlying implant damage. If fat transfer is being used to improve volume of a breast reconstruction, there is a slight risk of the implant shell being damaged. In such cases you may need to have the implant replaced
Are there any alternative treatments available?
Your specialist will discuss all treatment options available to you at your consultation.
What will happen if I decide not to have treatment?
If you decide not to have treatment, the appearance of your breast will remain the same
What sort of anaesthetic will be given to me?
You will be given a general anaesthetic. General anaesthesia is drug-induced unconsciousness. It is always provided by an anaesthetist, who is a doctor with specialist training. Unfortunately, general anaesthesia can cause side effects and complications. Side effects are common but are usually short lived; they include nausea, confusion and pain. Complications are rare, but can cause lasting injury: they include awareness, paralysis and death.
In addition local anaesthesia will be given to the part of the body where the fat will be taken.
If you are worried about any of these risks, please speak to your consultant.
Going Home
You will usually be able to go home the following day.
Pain relief and medication
The nursing staff will advise you about painkillers before you leave the hospital. Please tell the nurses what painkilling tablets you have at home. You will be advised to wear a compression garment for two weeks post-operatively. This is to help with swelling, bruising and for your comfort. Some people find the use of arnica also helps with bruising.
Your wound
Your wound will be checked at the time of your clinic visit by your consultant. If you have excessive pain or swelling at your wound sites, you should contact the ward, GP or the breast secretary.
Returning to work
You should be able to get back to work within few weeks after the procedure. You can self-certify for the first seven days of sickness. After this, a medical certificate (sick note) may be issued by your doctor to cover the expected time
Further Appointments
You will be given a clinic appointment when you are discharged from the ward.
Mastopexy (Breast Lift Procedure)
What You Really Need to Know About Breast Lifts
Click here for BAAPS guide for patients
Can I have a breast lift and not have implants?
A breast lift without implants works well in patients who are satisfied with their breast size but not satisfied with sagging and excessive overhang of their breasts and a low nipple position. A breast lift will reshape the breast, raising the nipple to a better position and reducing the overhang of the breast. The breast will not be smaller than it was before, just higher. There will be better fullness of the breast behind the nipple as the tissue is pushed upward and held in a tighter “skin envelope”. However, there is no way of reliably creating more fullness in the upper pole of the breast without using an implant. And since the scars of a breast lift are in the lower breast and hidden beneath a bathing suit, a lift will not tighten the loose skin of the upper breast; only restoring volume with an implant will fill out a truly deflated breast.
I just want implants. Why would I need a breast lift too?
Many patients who want to increase their breast size and fullness with implants want to avoid the additional scars of a breast lift. However, if the breast is too low and too overhanging past the crease under the breast, this skin and tissue will not be properly filled out by the implant and may have the appearance of “hanging off” the implant. This is also called a “double bubble” or “Snoopy” breast. This is because the bottom of the implant pocket is at this infra-mammary crease. If the breast hangs too low past this point, the implant will have little effect on filling it out. And if the nipple is low, it may become even more down pointing as it is too far below the midpoint or “equator” of the implant.
In summary, breasts implants do not lift breasts, they fill them out where they are. And if the breast hangs too low, they won’t even do that very well.
How can you tell if I need a breast lift in addition to implants?
When the surgeon examines you, measurements are made to assess where the nipple lies in relation to the fold under the breast, and how much breast overhang if any there is past this fold.
There are some patients whose breasts are “borderline” in terms of whether a breast lift is needed. The nipple may be somewhat lower than ideal, and there may be more breast overhang than ideal but not too excessive. In many cases a “dual plane” technique may be used in order to obtain a good result without the additional scars of a lift. This involves placing the implant under the muscle, as is usually done for better implant camouflage and a lower risk of capsular contracture, but releasing the attachment of the muscle to the overlying breast tissue a little to encourage the implant to “fill out” the loose tissue at the bottom of the breast. If this is successful, the nipple may look a little higher (even though it is not) as the bottom of the breast is filled by the implant. In this way, some of these borderline patients may avoid a breast lift. But if they want a higher breast or higher nipples, they will need a lift.
Why are there different types of lift and different scars with each one?
The breast lift with the least scarring is the periareolar or Benelli breast lift, which has a scar just around the areola and no vertical scar. In this lift a larger circle is drawn out from the areola, the top of this outer circle placed where the areola will be raised, and an inner circle is drawn within the areola (designed to reduce the size of a stretched-out areola). The skin between is removed, a purse-string suture is placed at the outer circle and cinched down around the inner, smaller circle, thus tightening the skin, reducing the areola size, and raising the nipple position.
Although most patients who need a lift want to avoid the vertical scar, there are serious limitations to this periareolar lift. If anything more than a very mild lift is required, the cinching down of this larger circle creates a gathering, puckered effect that leads to unsatisfactory scarring. Also, this tightening can lead to flattening of the breast shape that even an implant will not help counteract. (This lift is usually not attempted in patients without an implant, as the flattening effect and very minor lifting effect is not enough to obtain a good result.) Also, there is less control over the final size and shape of the areola, since late stretching of the areola can occur even with a permanent purse-string suture.
The vertical breast lift adds a vertical scar to this periareolar lift. This vertical scar has a very strong and effective shaping effect on the breast. A periareolar purse-string suture is still used, but closing the vertical incision reduces the size of the large outer circle and reduces the gathering effect. There is a difference of opinion among surgeons as to how effective this type of lift is at reducing significant breast overhang.
The anchor breast lift consists of a scar around the areola and a vertical scar, and adds a scar under the breast that allows very effective lifting and reduction of breast overhang. Moreover, the skin removal that raises the nipple to a better position and reduces the areola size does not require the dependence on a purse-string gathering suture; instead, skin is trimmed in a keyhole pattern than closes around the newly reduced areola with an exact fit. Thus the control over areolar size and shape is the most reliable, and the periareolar scar is of the best quality. Many surgeons believe this is the most effective breast lift with the best scar quality.
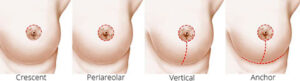
Can I have a breast lift and breast augmentation at the same time?
This is a controversial topic. Some surgeons never perform these at the same surgery, while others always do. Essentially, these two procedures can “work against” each other: breast augmentation expands the breast while a breast lift tightens the breast. You might think that you could place an implant and just “tailor” and trim the skin around it. Unfortunately, a certain amount of skin removal is required in order to lift the nipple to the correct position, close the defect where the nipple and areola used to be (and large areolas make this even tighter!), and adequately reduce the overhang of the breast. The tightness of this skin removal can restrict the size of an implant that can be safely placed, and this can be smaller than the patient desired. With too tight a closure, incisions can come apart, skin can lose its blood supply and die, healing can be prolonged, and the scars that result can be very wide and unsightly.
Another issue is the blood supply to the nipple. Dissecting a pocket for an implant can reduce the blood supply to the nipple, as can the dissection required to move the nipple higher as part of a breast lift. When performed separately, it would be extremely rare to have any blood supply issues; when performed together, this could tip the balance and loss or necrosis of the nipple and areola has been known to occur, especially with larger implants, tighter closures, and in patients with thinner tissues.
In general, patient who require minor lifts and have thicker tissues can often have both procedures performed at the same time, while patients with thinner tissues who need more major lifts may be safer having the lift performed first and the implant placed later. This staged approach takes a loose, overhanging breast that is not a good candidate for an implant, and reshapes the breast so that, once healed, it becomes a good candidate for breast augmentation.
No one wants extra scars that are not necessary, but many breast augmentation patients try to avoid a breast lift at all cost even when it is needed. This sets them up for a poor result and more surgical procedures in the future. Some surgeons will place too-large implants above the muscle in an attempt to fill out the loose skin and avoid the breast lift that the patient needs but does not want. Ultimately this may lead to even more tissue stretching and breast sagging, and require more complex surgeries to fix the problem. It is better to have a well-shaped breast with scars that generally fade nicely over time than an implanted breast with an unsatisfactory shape and contour.
Other Breast Procedures
Nipple inversion
Congenital asymmetry
Revisional surgery
Tattooing
Educational videos
Male Breast Conditions
Breast disorders are not confined to women. Men may also suffer with a benign over-growth of breast tissue called gynaecomastia. They may also get breast cancer, with many risk factors including medications and family history as the most common. Please see more information below from the Breast Cancer Care website:
Family History and Hereditary Breast Cancer
5% of all breast cancers may be due to hereditary factors. People with two or more first degree family members with breast cancer (or ovarian cancer), should seek referral for discussion and assessment of enhanced screening. I am happy to take direct referrals as well as GP referrals for women who are concerned they may have an elevated risk of developing breast cancer. Consultations will include a full breast examination and may include breast imaging e.g. mammogram. Please see below for more information from the Breast Cancer Care website:
Institute of Cancer Research (ICR) Family history assessment protocols (2015):
Skin Surgery
Breast disorders are not confined to women. Men may also suffer with a benign over-growth of breast tissue called gynaecomastia. They may also get breast cancer, with many risk factors including medications and family history as the most common. Please see more information below from the Breast Cancer Care website:

